Breastfeeding in the PICU
Our story this week comes from Brianna. Read on to hear how she pushed through and persevered to provide breastmilk for her son in a time when she felt otherwise helpless to do anythign for him.
I grew up in a home where breastfeeding was a frequent conversation topic. My mother is a lactation specialist, and it wasn’t uncommon for her to be helping a new mom with a breastfeeding question at the dinner table. When I had my daughter I knew I wanted to breastfeed, but our feeding journey was a roller coaster from the start. She wasn’t able to latch, she had tongue and lip ties, she fell asleep as soon as we started a feeding, and my milk supply was low. We had her ties reversed, but she still wasn’t able to nurse. I ended up pumping and bottle feeding for the three months of my materiality leave, and when it was time to go back to work we switched to formula. I felt guilty for being so relieved, but I truly hated pumping. It took me a long time to unpack the emotions I felt in those first few months. Ultimately I’ve come to learn that my worth as a woman and a mother isn’t defined by being able to breastfeed. Those months of pumping showed me that I was strong and determined, but they also taught me that my mental health is more important than where the milk comes from. A fed baby is a happy baby.
Fast forward to this past June when I was pregnant with our second baby. I told myself I was not going to put as much pressure on myself as I did last time. I almost didn’t even order a pump through insurance this time around, because I knew I didn’t want to pump again. I wasn’t going back to work because of COVID, so I figured I would breastfeed or bottle feed and that would be that. When our son Milo was born it was immediately different. He was rooting and latched right away. He didn’t have tongue or lip ties, and breastfeeding seemed to click. When we were discharged the next day I was feeling confident and thankful that feeding was looking easier this time.
Unfortunately the next several weeks were filled with frequent visits to the pediatrician. Milo lost 13% of his birth weight and was slow to gain it back. My milk was late to come in and once again my supply seemed low. I kept nursing, supplemented with formula for a few weeks, and by the time he was two months old he was finally gaining well and he was exclusively breastfeeding.
We were glad to be done with frequent doctor visits, until a couple weeks later when Milo woke up and something wasn’t quite right. He was fussy and he didn’t want to eat. He would cry every time I tried to get him to latch, but with a lot of effort he would finally nurse. The next morning he woke up, nursed once, and over the next couple hours we knew something was wrong. He didn’t have a fever, but he was unable to nurse and he seemed lethargic. We saw the pediatrician who believed he was constipated and dehydrated. She sent us to the local emergency room, and we were admitted. When we got to the ER I realized since I hadn’t nursed him all day, I needed to pump. I called my husband to retrieve the Spectra pump I had begrudgingly ordered and stuck in the closet. I pumped that evening and tried to syringe feed Milo, figuring the next day he would nurse again once he was feeling better. However, the next morning he was worse. He was unable to swallow and was making this awful, low, whining cry. He was more lethargic than the day before, and I knew something was very wrong. We were transferred, via ambulance, to a nearby children’s hospital. As the day went on I watched my sweet baby get sicker and sicker. He could not swallow, he could not move, he could hardly cry. At one point, his oxygen saturation dropped, and the pediatric team initiated our transfer from the peds floor to the pediatric ICU. When we arrived on the floor Milo was immediately evaluated by the PICU team. The attending, who I will forever be grateful for, examined him for several minutes and then said, “I think this is botulism.”
My husband arrived just as the team was leaving (up until this point I had been by myself due to COVID policies) and the attending reviewed his plan with us. Our son was presumed to have infant botulism, and the attending recommended we begin the treatment immediately. The drug used to treat botulism is an orphan drug called BabyBIG. It’s only made in California, and each dose must be made and transported as needed. Testing to confirm botulism takes several days, so it is recommended that treatment begin without confirmation when botulism is suspected. The team requested the dose of BabyBIG right away and it arrived in New York roughly 12 hours later. Milo received the dose of BabyBIG almost immediately, and then we just had to wait and hope the diagnosis was correct.
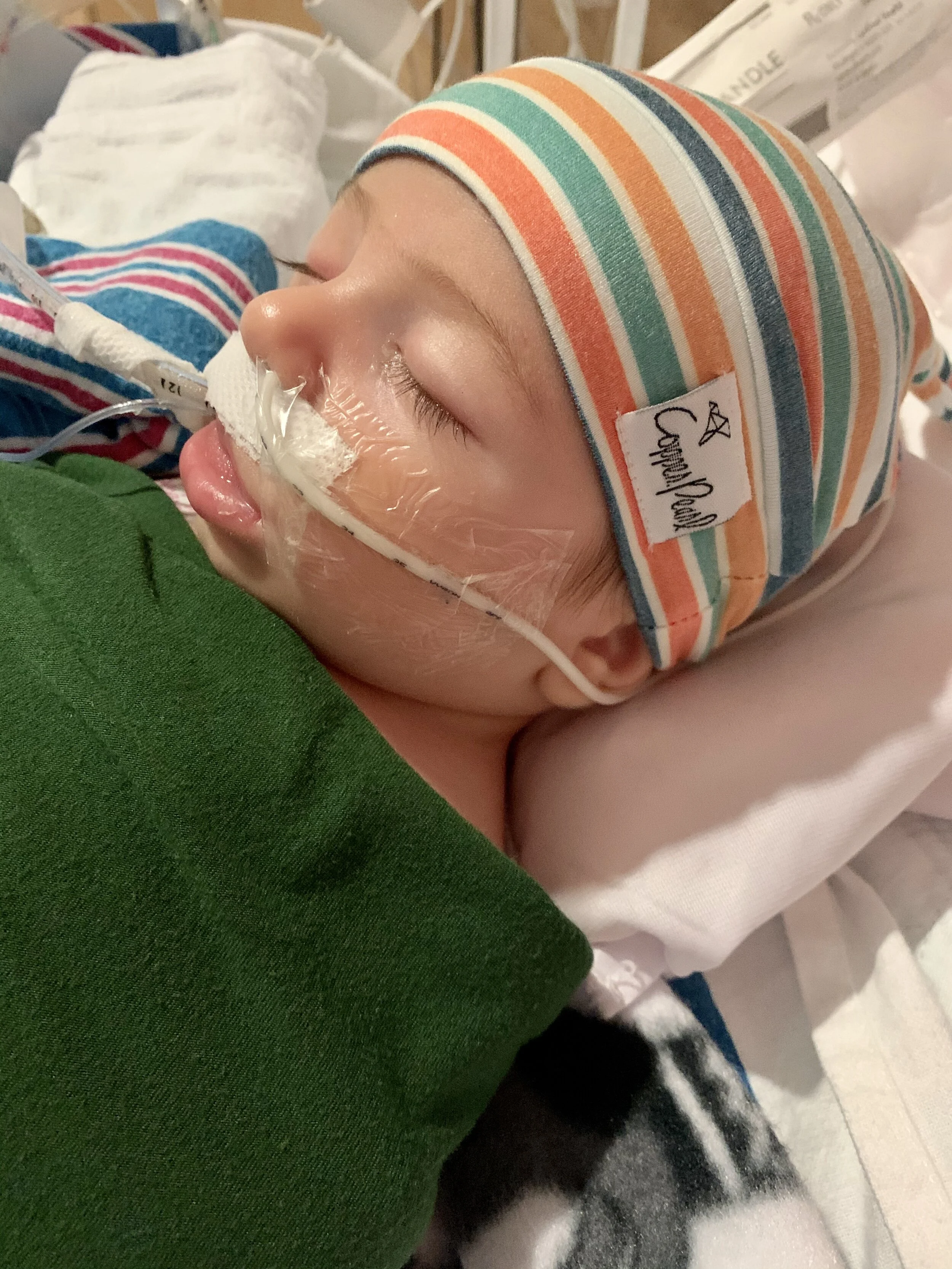
Over the next several days the PICU team ran test after test to rule out other diagnoses (meningitis, genetic disorders, metabolic disorders, etc.) while waiting to confirm botulism. During this time, our son was intubated, sedated, and a feeding tube was placed. Botulism toxin blocks nerve endings from being able to contract muscles, so as the toxin moves through the body it slows digestion, motor movement, swallowing, and breathing; essentially paralysis. When the feeding tube was placed, it was my first chance to feed him in days. My milk supply had tanked, as I was mainly pumping for comfort, but something ignited within me and I was determined. Sitting in a PICU room with a sick baby makes you feel helpless, but pumping was something I could do. He could still have breast milk through that feeding tube. So I got to work. Family members made and dropped off lactation cookies, my mother sent supplements, I got appropriate sized flanges from the hospital's lactation consultant, and I pumped. I pumped every 2-3 hours for the next week and a half, and that precious milk went right into the kangaroo feeding bag connected to his NG tube. As exhausted as I was, I was glad to be able to do anything to take care of him in such a helpless situation.
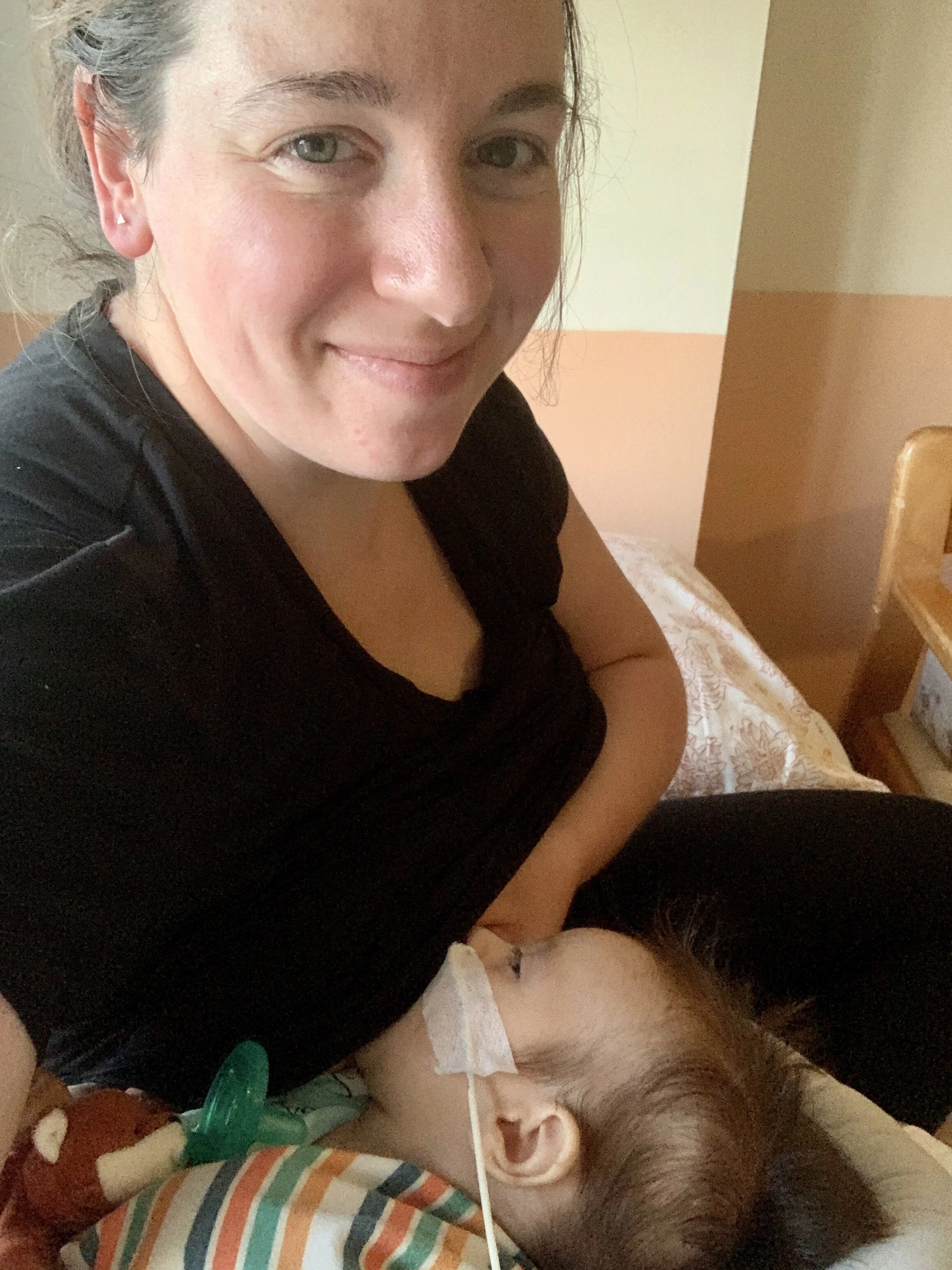
Four days after receiving the BabyBIG, Milo was showing progress. He was beginning to move his arms and legs. The next day he opened his eyes. A couple days later he was breathing on his own. Slowly his suck started coming back. It was incredible watching everything he lost be reversed as his muscle strength and movement were restored. On the day he was extubated we were finally allowed to hold him again, and that was spectacular. Soon after, he was cleared for non nutritive nursing, so I would pump and then he would latch and essentially “practice nursing” while receiving his NG feed. It was exhausting, but seeing progress each day helped us move forward.
Toward the end of our stay he completed a fiberoptic endoscopic evaluation of swallowing (FEES) to determine if he was safe to resume oral feedings. He passed, but they wanted him to start off with bottle feedings. Those feedings were challenging because he wasn’t a bottle fed baby and he didn’t have the stamina to complete a bottle feeding. After a day of bottle feeding attempts, and some advocating on my part, they cleared him for nursing instead. Once again I felt relief as part of my breastfeeding journey, but for totally different reasons. My baby was back in my arms nursing and my hard work to restore my milk supply had paid off.
Many babies with botulism are discharged from the hospital with their feeding tubes, as the swallow can be impacted for a variable amount of time, but after two days of successful nursing Milo’s feeding tube was able to be removed. While that was an exciting moment, nothing compared to the following day when we were discharged, two weeks to the day were admitted.
I’m so in awe of Milo's strength and resiliency. While we were in the hospital several people told us, “he won’t remember any of this.” True, he won’t, but we sure will. I will never forget seeing him in that hospital bed, and I won’t ever take for granted the ability to hold and feed my baby. I’m so proud to have persevered with pumping and that our breastfeeding journey can continue. There will still be hard days; we are parenting a baby and a five year-old after all, but thankfully this little guy has smiles in spades.
What do you think about Brianna’s story? We think she did an incredible job at doing the best she could for her babies! Thanks for sharing Brianna!
Would you like to share your breastfeeding story our blog? Submit it here!